Gastrointestinal (GI) Bleeding: Warning Signs, Causes & When to Seek Help
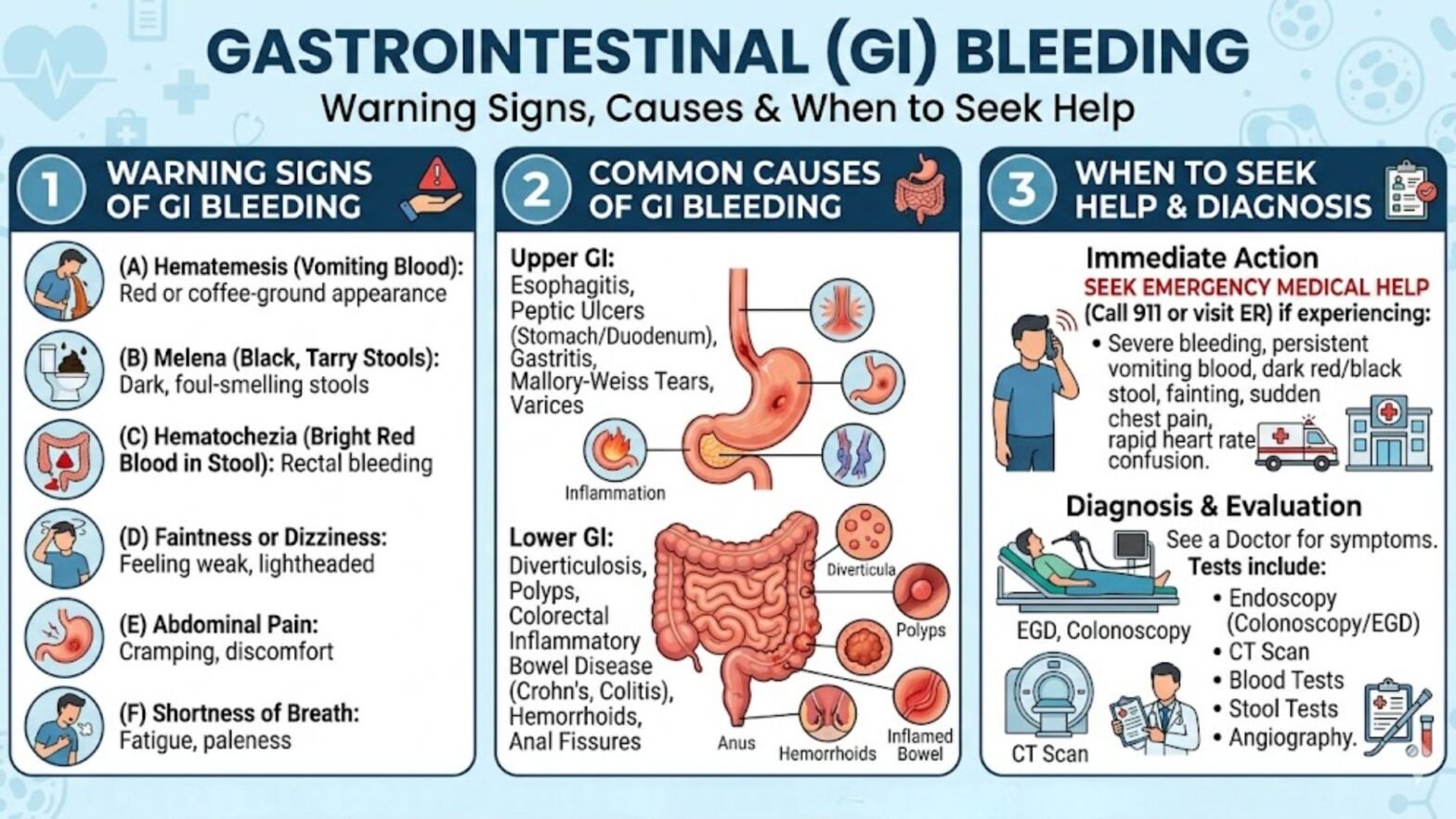
Gastrointestinal (GI) bleeding is a serious medical condition that should never be ignored. While it may sometimes appear as a minor issue, it can signal underlying diseases that require immediate diagnosis and treatment. Early detection can be life-saving and significantly improve outcomes.
In this blog, we’ll explore the causes, symptoms, and treatment options for GI bleeding—and when it’s time to consult an expert.
What is Gastrointestinal (GI) Bleeding?
GI bleeding refers to any form of bleeding that occurs in the digestive tract, which includes:
- Esophagus
- Stomach
- Small intestine
- Large intestine (colon)
- Rectum
The bleeding can be visible (overt) or hidden (occult) and may range from mild to severe.
Common Causes of GI Bleeding
Understanding the root cause is crucial for proper treatment. Some common causes include:
Upper GI Bleeding Causes:
- Peptic ulcers
- Gastritis
- Esophageal varices
- Acid reflux-related damage (GERD)
Lower GI Bleeding Causes:
- Hemorrhoids
- Anal fissures
- Diverticulosis
- Inflammatory bowel disease (IBD)
- Colorectal cancer
Warning Signs You Should Never Ignore
Recognizing symptoms early can make a critical difference. Watch out for:
- Blood in stool (bright red or black, tarry stools)
- Vomiting blood (may appear red or coffee-ground like)
- Unexplained weakness or fatigue
- Sudden dizziness or fainting
- Abdominal pain or cramping
- Drop in blood pressure (in severe cases)
⚠️ Even mild symptoms can indicate a serious condition—don’t ignore them.
When is GI Bleeding an Emergency?
Seek immediate medical care if you experience:
- Heavy or continuous bleeding
- Severe abdominal pain
- Rapid heartbeat or low blood pressure
- Fainting or confusion
These may indicate life-threatening internal bleeding.
Diagnosis and Treatment Options
A specialist will recommend tests based on symptoms, such as:
- Endoscopy or colonoscopy
- Blood tests
- Imaging scans
Treatment depends on the cause and severity:
- Medications (to reduce acid or inflammation)
- Endoscopic procedures to stop bleeding
- Surgery in severe cases
Early diagnosis ensures less invasive treatment and better recovery.
Prevention Tips
While not all cases are preventable, you can reduce risk by:
- Avoiding excessive use of painkillers (NSAIDs)
- Managing acid reflux effectively
- Limiting alcohol consumption
- Eating a balanced, fiber-rich diet
- Getting regular health check-ups
Frequently Asked Questions (FAQs)
1. Is GI bleeding always visible?
No. Some cases are occult bleeding, which may not be visible but can cause anemia and fatigue.
2. Can GI bleeding stop on its own?
Minor cases may stop temporarily, but the underlying cause still needs medical evaluation.
3. Is black stool always a sign of GI bleeding?
Black, tarry stool (melena) often indicates upper GI bleeding, but certain foods or medications can also cause discoloration. A doctor’s evaluation is essential.
4. Can stress cause GI bleeding?
Stress alone doesn’t directly cause bleeding, but it can worsen conditions like ulcers or gastritis.
5. Is GI bleeding linked to cancer?
In some cases, especially in older adults, GI bleeding can be a sign of colorectal or stomach cancer. Early screening is crucial.
Don’t Ignore the Signs—Act Early
Gastrointestinal bleeding is not just a symptom—it’s a warning signal your body is sending. Ignoring it can lead to serious complications.
📞 Take Action Today
If you or your loved ones are experiencing any of these symptoms, don’t delay.
Consult Dr. Shivam Vatsal Agarwal
Director & Head – Surgical Oncology & Robotic Surgery
Metro Cancer Institute
Early diagnosis saves lives. Get expert guidance and the right treatment at the right time.

